MANAGING YOUR HEALTH
There is a misconception that because there are no approved drug treatments for FSHD then there is nothing you can do.
While it is true that at the moment there has been no treatment that has been shown to stop progression or reverse damage caused by FSHD. There are many treatment techniques used at the moment that are applicable to FSHD and may provide some help and improve quality of life.
It’s important to note that many of the therapies listed below have little empirical evidence supporting their use in FSHD. This just means that studies have not been done on these treatments. Because FSHD is so variable it is difficult to predict what treatments may work for you. An individualised plan developed in collaboration with a health professional you trust will help you decide on the best treatments.
Physiotherapy
There are many different techniques and types of physiotherapy. They won’t all work for everyone and you may have to engage in some trial and error to find a practitioner and a technique that works for you.
It’s important that you find a practitioner who has some experience in neuromuscular conditions, or degenerative conditions. This is because much physiotherapy is focused on recovery. With FSHD, as with many chronic degenerative conditions, recovery is not the goal. Maintenance of condition, improving or maintaining balance and supporting fitness is the aim of therapy.
It may be helpful to speak about your goals and your physical limitations before you start on treatment planning with your physiotherapist. This may help avoid frustration.
Finding a practitioner who is suitably trained and experienced may be challenging. If you are currently seeing a neurologist ask for a referral to a physiotherapist, or for some suggestions. You can also ask your GP, nurse or other care worker if they know anyone in your area who is trained to work on neuromuscular disease.
We also have a forum where people with FSHD can post the details of health professionals they have found supportive and helpful. You can also post in the forum asking for suggestions of who to see, or add your own.


Hydrotherapy
There are no trials looking at the benefits of hydrotherapy for FSHD. However, hydrotherapy does assist mobility and can be an efficient means of exercising. Many physiotherapists will offer hydrotherapy sessions.
Massage
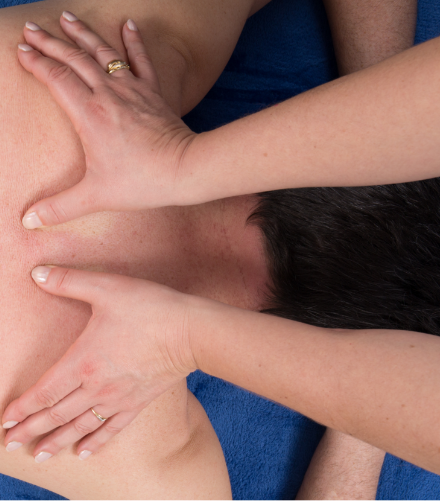
Massage may be effective for managing pain and help with stretched and strained muscles. Speak to your health professional about massage, they may be able to refer you to a good therapist in your area, or direct you to therapists who may be covered by your health insurance.
Exercise
There have been a number of studies into exercise for FSHD. Unfortunately, these studies were short with a small population and it is therefore difficult to extrapolate the results to a recommendation for treatment. However, a recent review concluded that the evidence suggested exercise for FSHD is not harmful. There are more groups around the world performing studies on exercise for FSHD so hopefully in the future we will have some more concrete evidence.
Exercise does have a number of benefits so the lack of evidence should not deter you from speaking with your health professional about designing an exercise program. There are a few considerations you should take into account while planning an exercise program.
There are two types of exercise, aerobic and resistance. Aerobic exercises include activities like running, cycling and swimming. They temporarily elevate heart rate and breathing rate. Resistance exercise includes activities such as lifting weights. They build strength in the muscles.
While aerobic exercise has not been associated with negative effects, there are a couple of concerns with resistance exercises that may leave people prone to injury. The first is the differences in strength in different muscle groups. For example, let’s say your bicep muscle in your arm does not have any significant weakness, but the muscles surrounding the bicep do. Then weight training your arms may lead to overuse or stretch injury in the weaker muscle. The second concern is fatigue. For people with significant weakness simply performing activities of daily living may be exercise enough. Further stressing the muscles with weight training may result in overuse injuries.
If you would like to engage in a resistance training program it is best to do it with direction and support from a physiotherapist with experience in neuromuscular disease and an exercise physiologist also with neuromuscular disease experience.
Aerobic exercise like swimming, using a stationary bike and walking will improve your overall fitness with less risk of injury.
Before embarking on any exercise program please consult your health professional.
Surgical management
There are a number of options for surgical management of FSHD that are mainly concerned with fusing bones. The basis of these surgical methods is to help treat the instability created when muscles weaken.
One of the most common ones is scapular fixation. The scapular is also called the shoulder blade and sits on the back. Often in FSHD progressive weakness in the muscles that hold the scapular against the back and attached to the arm, leads to winging and eventually an inability to lift arms. During the procedure the scapular is attached to the rib bones that lie underneath it. This can improve the function of the shoulder.
There are other surgical techniques that may provide some help. However, surgery does not always result in significant improvement and it’s important that you have considered all the risks and benefits with your health professional before deciding on a surgical treatment strategy.
Respiratory support
Other muscular dystrophies are associated with breathing difficulties because eventually the progressive weakness spreads to the muscles that control breathing. This is not a common complication of FSHD. However regular monitoring of breathing function is recommended especially as you may not realise you have poor breathing function.
Difficulty breathing means there is not enough oxygen getting to your tissues. This can exacerbate the negative effect of FSHD on your muscles.
Breathing problems during sleep is also not a common complication of FSHD, but it can happen. Symptoms include disturbed sleep, morning headaches, daytime fatigue and sleepiness. It is relatively simple to diagnose and treat night time breathing problems. Some people may respond well to position therapy to help you sleep in a position that limits any obstruction to breathing. Non-invasive ventilation is also an option.
Orthotics, walkers, crutches and the chair
When many people think about muscular dystrophy they think about people confined to a wheelchair. While it is true that many people with FSHD do use a wheelchair for mobility the idea that they are confined to it is misleading. Some people may have lost the ability to walk and therefore need the chair to get from a to b. Others may use a chair for long distances to prevent fatigue. Some people may have significant foot drop and therefore use the chair because it allows them to get around while preventing falls and fractures that might seem them completely reliant of the chair.



